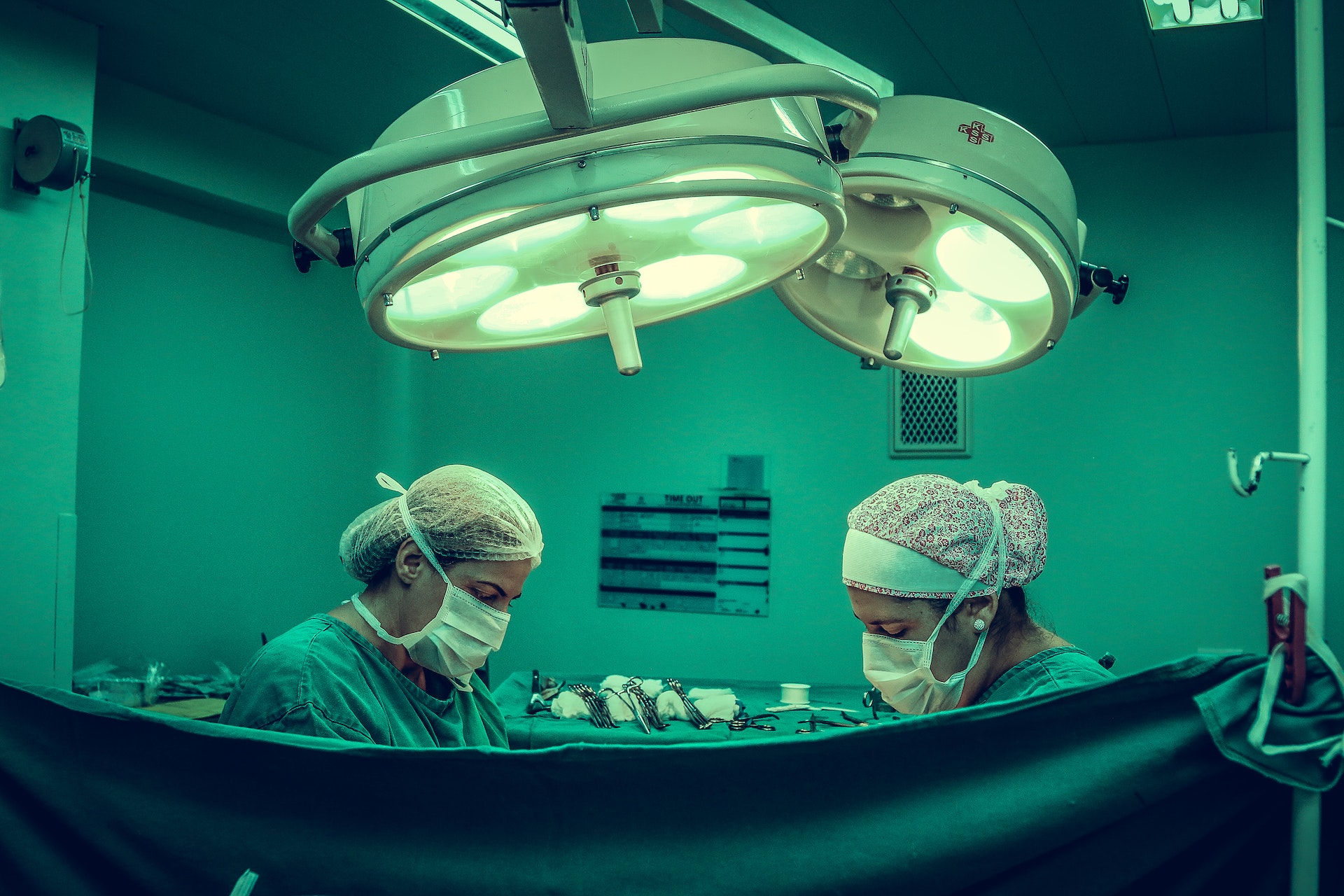
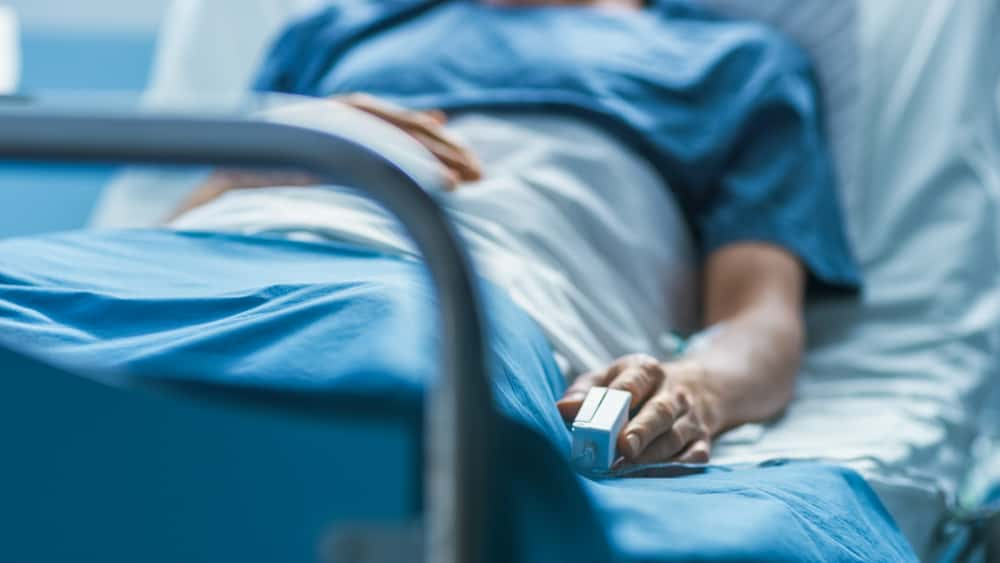
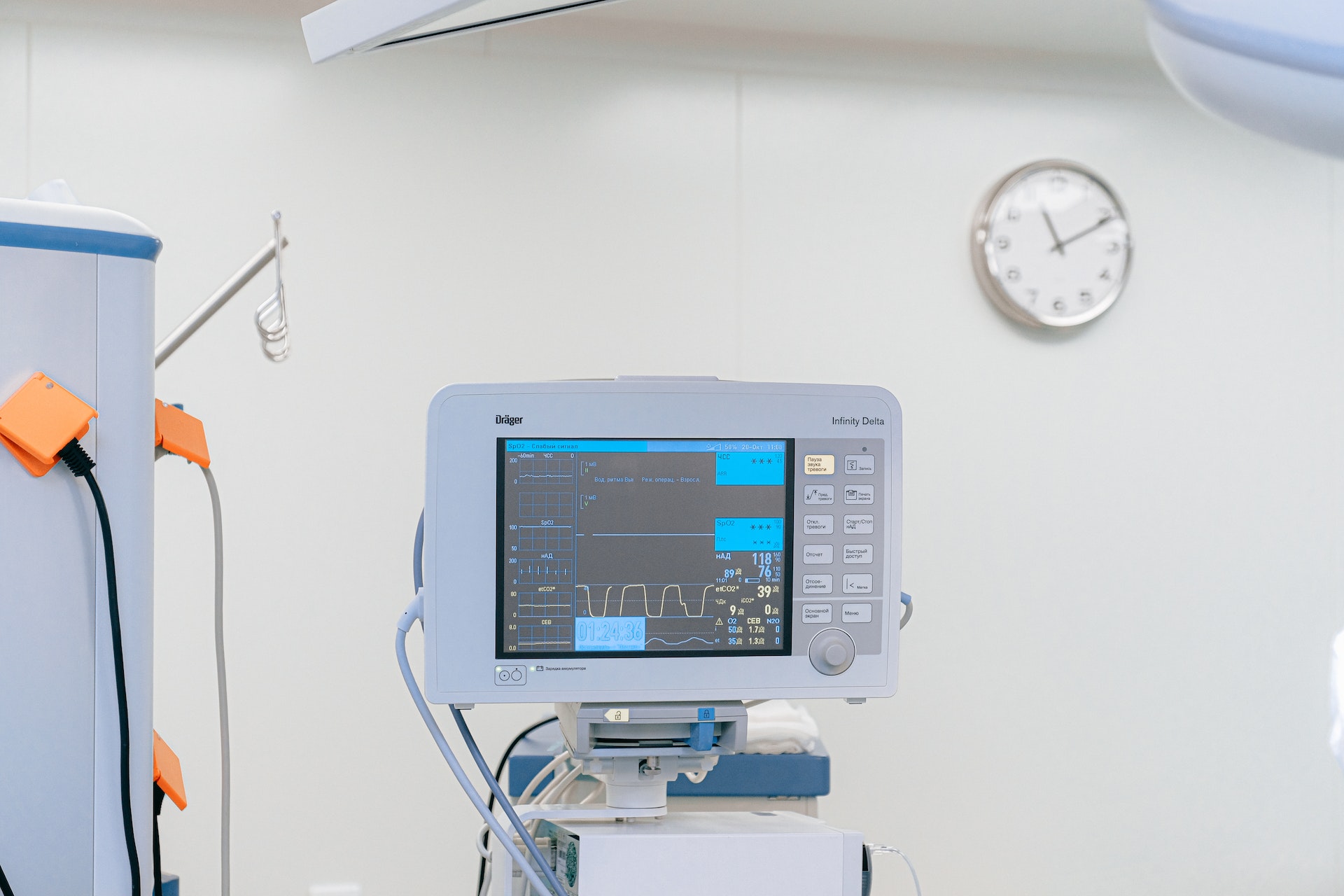
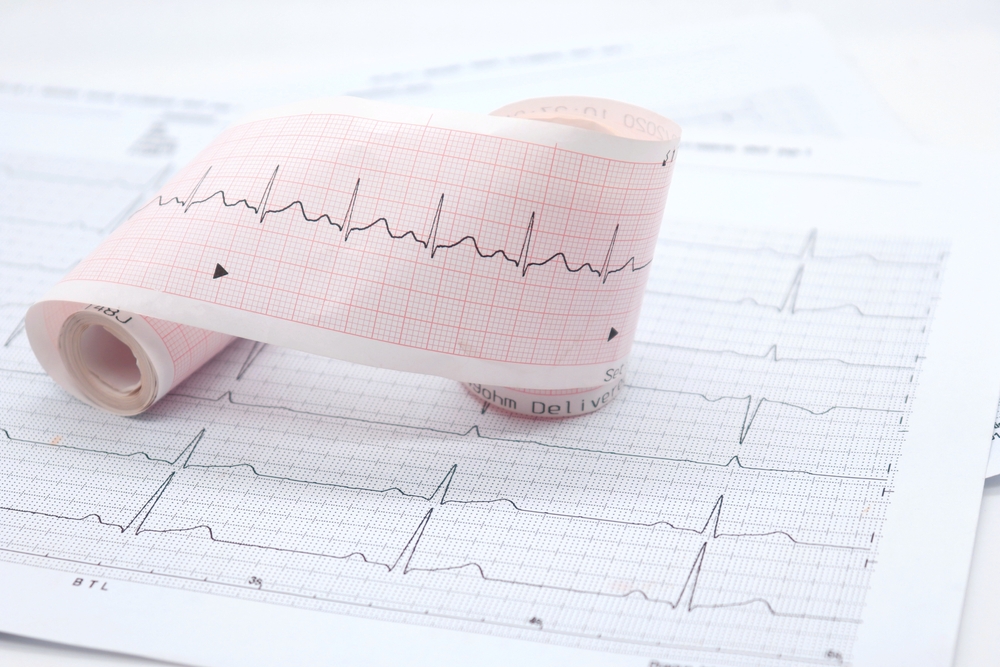
Doctors and medical professionals see patients in all sorts of conditions. There are times that even they are stunned that the person in front of them is still living and breathing. These Redditors share their stores of people who should have been long gone yet weren’t. Miracles indeed happen every day.
1. What A Fall!
We were the closest hospital, so they brought a civilian in. His safety gear failed, and this guy fell 128 feet from a communications tower. It had rained the night before, and he fell into a marshy puddle of high grass, flat on his back. When I took a look at him, I couldn't believe what I was seeing. He had a concussion and whiplash. No broken bones, but the bruises that covered his body from head to heel were something to behold. He spent a week in the hospital before he could move comfortably.
2. Are You Kid-neying Me?
A friend of mine was feeling unwell for days. He'd go to work, feel exhausted, come home, sleep 13 hours, and repeat. Finally, he got to feeling so bad he decided to go to the ER. He drove himself at around 3 AM. He got out of the car, and the security guard said, "OH MY GOD", and ran to get him a wheelchair. ER admissions also said, "OH MY GOD", and got the ER doc.
The ER doc noted my friend was quite yellow. They ordered blood work, and when it came back, the ER doc didn't believe it and had it done again. When the second round came back, the doc asked my friend for next of kin information. My friend said, "You can't call my mom, it's 4 AM", and the doc said, "Your kidneys have completely failed."
"We are going to send you upstairs and give you a pint of blood and an hour of dialysis, and we need to know who to call if you still don't make it. You should have been [gone] a month ago". He got a kidney from his sister and is still doing well today. Apparently, the kidney was as close a match as one can get, and he should live an essentially normal lifespan.
3. The Sweet Life
I had a patient who was already blind from diabetes and lost some toes and part of a foot. I checked their blood sugar, and it was 45. I thought I must have made a mistake. The normal range is 4–7. I checked it again, and it was 45. This patient had no symptoms of hyperglycemia. He just took his insulin pen, cranked it, and self-injected. I had to wait around a bit to see what would happen, but eventually, we left, and he ended up being totally fine. Most home glucometers don't go past 30. I was with my trainer nurse, who was dumbfounded.
4. Everything But The Kitchen Sink
As a lab tech, I had one I dubbed "Everything Guy". He was complaining of a sore stomach after coming home from overseas, so he got the usual, "what were you doing"? questions. He was in West Africa and didn't bother to get antimalarials and didn’t have any vaccines. He admitted to eating bushmeat and also said he thought it was undercooked.
He drank water from a "local source", which turned out to be directly from a river, without filtering it. The river was apparently badly polluted. He also hired ladies of the evening while there and didn't use protection. He basically did everything you shouldn't do on holiday and used it as a checklist.
5. Blood On Our Hands
I had a patient who had just delivered. She pushed for more than four hours before ending up with a C-section. We got back to the room, and I pushed down on her belly to check the bleeding. It was a little excessive, so I called the doc. He came in, and she had minimal bleeding because that’s how it goes. The blood pressure monitor went off; it was in the 60s.
I did another fundal and had nonstop tennis ball-size clots coming out. Luckily the doc was at the nurse's station, and someone showed him the blood pressure. He came into the room as I was doing the fundal and immediately called a massive transfusion protocol. We ended up in the OR, giving her so much blood. He placed a tamponade balloon, and we went to PACU to finish the recovery.
It was just one other nurse and me. Everything was going well for a bit, but then suddenly, everything went wrong. There was more bleeding than normal in the drainage bag, her lips were blue, her face was super white, and her blood pressure reading was in the 50s. The doc sent his resident to check it out, who said it was fine and to give more blood. I ended up calling the anesthesiologist and asking him to come to assess.
He was known for being rude, but he came in there and immediately called the OB and yelled at him to get in there immediately. I had a lot of respect for him after that and was really grateful he hadn’t dismissed me. We ended up back in the OR, and she ended up needing an emergency hysterectomy. The doc described her uterus as being a paper bag.
I came from the ICU and was used to patients that looked terrible, but I really thought this lady was going to code and lose her life. She ended up losing about three liters of blood, was intubated, and was in the ICU for a few days. I never went to go see her again because I was so mortified by what had happened. I was newer to labor at the time and kept feeling like I made a mistake somewhere.
6. The Gall Of It All
The doctor who saw my mom said he had no idea how she was alive. Years ago, my mom was having gastrointestinal problems. She had incessant stomach aches and was bound up something awful. After three days of not being able to poop, she went to the doctor to get checked out. After a thorough examination, the doctor determined that her gallbladder needed to be removed immediately.
The next day, after the surgery, my mom came to and saw the doctor standing over her, and he wasn't happy. "Your gallbladder was [gone]," he said. "Like, [gone, gone]. In fact, it was completely gangrenous. Had you waited another day to see me, you would've [passed]. Had it ruptured during surgery, you would've [perished]. That was the worst, most stress-inducing surgery I ever had to perform in my 20-year career. No offense, but I hope I never see you again", and he walked out of the room.
7. A Change Of Protocol
The CPR algorithm changed about a decade ago from ABC (airway, breathing, and circulation) to CAB (circulation, airway, breathing). This means that instead of opening the airway and giving rescue breaths first, we begin doing compressions first. The first time I used the new version was at a witnessed coronary. I happened to be at the patient’s bedside when their rhythm changed and was, therefore, able to start treatment immediately.
The patient became unresponsive and pulseless, and the rhythm showed ventricular tachycardia. I began chest compressions, and the patient raised their arms and tried to punch me. Confused, I paused and checked for a rhythm and pulse and assessed their alertness. The rhythm was indeed pulseless ventricular tachycardia, and they immediately rolled their eyes back and went limp. I must have gotten on the chest so quickly that they hadn't had time to lose brain perfusion. It's never happened since.
8. MRSA Almost Did Me In
Years ago, I went into the ER to get a cyst lanced open. Three weeks later, I felt pain in my back. I went back to the ER, and they found nothing; they only did X-rays. I felt weak leaving, so I went home and crashed on my couch. I woke up hours later, tried to get up, and fell. I went down fast. I called an ambulance and went to the hospital.
I sat for six hours until, finally, someone came to check me out. I had a 105°F fever! They immediately rushed me into an MRI, and lo and behold, I had MRSA inside my spine. I was rushed into surgery and now live in a wheelchair. My T5 to T11 were fused. The doctors said if I waited one more day, I wouldn't be here. I did 16 weeks of Vancomycin thru IV, three hours twice a day! I’m truly lucky to be alive today.
9. Too Cold For Comfort
I had a patient with an internal temp of 75°F. He was drowsy but fully alert and oriented. He was found in a river embankment in the middle of the winter. He had been lying there overnight before he was found by a dog walker. We didn’t believe the equipment when it told us 75 degrees, so we repeated it with a rear-end thermometer.
Then a different rear-end thermometer, and then a rear probe attached to the bedside, and a medi-therm system. They were all consistent, and after several hours of heating measures, we got their internal temperature up to 90 degrees before they went to the ICU.
10. Eat Up!
When my son was a day old, the nurse came in to check on him. She couldn't get a temp, so she went and got a new thermometer (digital). Same as before, no reading. She was puzzled, so she brought him out of the room and put him under a heat lamp. After a while, his temp registered. They knew something was terribly wrong. They tested his blood sugar, and it was a two.
It started to get very scary for everyone, and he went down to the NICU for the next two weeks. It turned out he had a genetic disorder called MCAD. His body cannot process medium-chain fats. Hence, he cannot fast, ever. His body will use the reserves of sugar, but once they are depleted, he could crash and go into a diabetic coma. This is what happened the day he was born.
He wouldn't feed and didn't want a bottle. So we learned of his condition the hard way. The first one and a half years of his life were tough, as he had to wake up and eat every few hours. My wife and I never had a full eight hours of sleep for almost five years. We landed in the hospital when he was vomiting from the flu many times. If he can't keep anything down, he must go on a sugar drip.
But today, he is 11 and healthy—5'8” and 155 lbs—a big, strong, solid boy. He has no long-term disabilities from the sugar crash. The condition has never presented itself again, but we do make sure he always has enough calories. My only concern is when he is a teenager or young adult. Fasting during a hangover is OK for most, but not for him.
11. Snaking Along
We once received a patient who was bitten by a rattlesnake TWICE. He only managed to get to the emergency ward three hours after being bitten. Then, to make things worse, we only managed to get the correct antivenom flown in one hour after his arrival. He now works at our hospital as an admin clerk and is healthy as ever.
12. Holding On For Dear Life
During my EM rotation, a guy had a road accident. He had deep flesh wounds, and his intestines were out, around 40% of his face was scraped off, one eye was out of the socket, the right forearm had ripped-off muscles, and you could see the bone. The miracle was that the bleeding somehow had stopped when I came in. I saw his chest moving and him holding his intestines. I was like, “Yeah, wow, this guy is alive”. We helped him, stitched everything back, his face was reconstructed, and now he is alive and well.
13. Against All Odds
I work in the public health field, and I’ve had a few patients to track down that I honestly had no idea how they survived. One had a laundry list of issues—Hep A, B, C, endocarditis, a messed up mitral valve, AIDS, abscesses, and disseminated MRSA in their bloodstream. I was required to gown up with a mask, gloves, and the whole nine yards just to be in the room with them.
I quickly found out they were in no state to answer any questions I had. I found out later they were transferred for open heart surgery to a different hospital after—no lie—attempting to check out against medical advice (AMA). At the second hospital, they had completed surgery and were finally somewhat on the mend. Their parents checked them out—again AMA—to make the multi-hour drive back home.
I was absolutely flabbergasted. I figured there was no way they’d even make it home. Lo and behold, they cropped up again in a public health investigation a year later, alive. I was shocked they had survived that long.
14. Eternal Slumber
I’m a sleep tech, and I had a middle-aged patient whose oxygen fell all the way down to the 40s and who was having central apneas for over a minute. He spent more time not breathing while asleep. It was no wonder he complained every single day that he didn’t feel alive. I couldn’t believe it, so I tried a bunch of other oximeters and different hands/fingers, and they were all incredibly low while he was asleep.
15. Preemies Pulling Through
I used to work in obstetrics and in the preemie ward. I've seen some extremely premature babies that looked like they were barely hanging on. They have tiny heads, maybe two inches from the chin to the top of the cranium, purplish/reddish translucent skin that looks paper-thin, eyes closed, not responsive, limbs smaller than a finger, and always extremely skinny.
They often face lifelong problems due to being born so prematurely. I remember once asking the doctor why we even bother at that stage since it looks so hopeless, and in some cases, is. She said, and I remember very well, "The preemies that were hopeless cases 20 years ago now live normal lives, so that is why we keep on pushing".
16. My Life Almost Went Down The Toilet
I had a hemorrhage I didn't know about. I had seen some blood while wiping, that was a bit more than I chalked up to wiping too hard. I went to a physician, and he checked my rear and told me I had hemorrhoids that I had probably agitated. He recommended I use baby wipes and Preparation H. Two days later, I started feeling very nauseous with a nasty headache.
I slept right up until it was time to go to work and decided I shouldn't call in sick. That mistake nearly killed me. About five hours into my shift, I go to take my break and use the restroom. The moment I pushed, I passed out and fell off the toilet, to be found by my coworker much later. EMTs loaded me up and started taking my vitals. My O2 levels were low, and when we got to the hospital, they rushed me through the back and into a room.
They said I needed blood pronto, and I remember passing out again. The next thing I woke up to was an RN throwing my curtain open and shouting, "WHY ISN’T HE HOOKED UP YET"?! Apparently, the ball was dropped somewhere between getting my blood type and the blood being dropped off. So I sat there for over 45 minutes needing blood, and that RN was madder than heck.
I finally got hooked up, and I took three pints of blood, stayed overnight, and needed another pint by the next afternoon. The hemorrhage was found, microsurgery was performed, and I've been fine ever since. The same RN came to see me after my surgery and told me she was terrified I wasn’t going to make it when the EMTs handed over my vitals when dropped off.
17. A Stroke Of Luck
A young woman in her 30s had a stroke. She clotted off the basilar artery, the big artery in the base of the brain that supplies all of the "primitive" functions, like breathing and awareness. I found out about her a day after the event. This, by the book, is a hopeless case. She was literally already gone. But, because she was young, they prevailed upon me to do something.
I poked a catheter into her groin artery, then snaked it up to the blocked artery in the base of her brain. I infused a clot-busting medication into the artery for about 12 hours (tPA). I re-checked, and the clot was gone. She woke up the next day. After a month, she literally walked out of the hospital. It was the most miraculous thing I've ever seen.
She sent me a nice card a month or so later. It bothered me that her handwriting was better than mine, even after her stroke, but I was pretty happy.
18. Glop In His Gams
My dad has a blood condition that makes him prone to clotting, and it has sent him to the hospital several times now. The most recent case was this. He had started doing nightly runs, raising money for a charity, and every time he came home, he'd be more and more puffed out with a really sore leg. He mostly just thought it was muscle cramping until, at one point, my mom just told him to check it out at the doctor's.
The doctor immediately told him to go to the hospital as soon as he described it. The hospital took him in, sent him for an MRI, and, in the nurse’s words, “They stated it was the largest blood clot they ever saw in a person that was still breathing”.
19. Marfan’s Maimed Him
I was a cardiovascular tech. I was doubling as a special procedures tech in radiology when a healthy young man in his 20s who was visiting a friend collapsed in our CCU. He had lost femoral pulses and, overall, was suddenly very critically ill. We were asked to do an aortic angiogram to define his anatomy, and all arterial access was occluded.
We finally got a catheter in his left axillary artery and managed to get a picture of his total aortic dissection that began at his aortic valve, spiraled down, and occluded his right renal and most of his iliac arteries to the femoral. We did what we could to stabilize him and sent him to Houston, where he was grafted and lived.
I saw him about two years later when he was back at our shop for a checkup. He was scarred from his neck to his knees; there was a lot of plastic in there! He had unsuspected Marfan syndrome, and it almost ended him. I never saw anyone else with close to that much vascular damage who survived. I wasn't all that aware of Marfan syndrome back then, and now every time I see long skinny digits, I remember that guy.
20. Black Market Bacteria
A 23-year-old female came in with sepsis after a kidney transplant on the black market. She had been on the transplant list but had not yet received a match, so I guess her parents decided to take her fate into their own hands out of desperation. The parents wouldn’t tell us where they had been to acquire it, but the patient was septic with a strain of bacteria called New Delhi metallo-beta lactamase (NDM).
This kind of bacteria produces carbapenemase, an enzyme that digests a wide range of β-lactam antibiotics, including carbapenems, which are basically our last resort of antibiotics for the treatment of infections caused by resistant strains of bacteria. So, the patient was being pumped full of our best antibiotics, and this bacteria was simply digesting them. The patient then got a secondary pseudomonas infection in both eyeballs and had to have them removed. Pseudomonas is a nasty bacteria and one you don’t want in your eyes.
21. Padded Bliss
There was a youngish female—early 20s maybe—around 400 lbs who was in a high-speed motor vehicle collision. Her car was torn in two, and she was ejected around 100 feet. She landed against a telephone pole. When the authorities showed up, they assumed she was gone, but she wasn’t—just trashed. Her massive body fat had protected her from pretty much any injury. I think she broke a few bones but was fine.
22. Gut-Wrenching Accident
Back in my surgical days, I was a resident on my trauma rotation. A really nice young guy comes in via EMS. He'd been working on a factory site doing work high up on a tower. He was climbing his way down—about halfway—when he heard commotion overhead, and someone shouting, “Watch out”! There wasn't any time for him to react.
He felt something strike the back of his neck. He managed to stay calm, reached around, and realized a large piece of metal was embedded in him. His medic training engaged. He calmly climbed down the rest of the ladder, sat down, and asked someone to call an ambulance. It was a wrench 36 cm (14 inches) long, but the non-wrench end was a pointed pick ax-type tool.
That was what was embedded in him. It was nestled nicely against C3/C4 (middle of the neck). All we could get were X-rays because there was too much metal artifact for a decent CT scan. We couldn’t see any fractures. It was a fully intact neuro exam. A rock star of a spinal surgeon just decided to yeet it out. The guy had a few stitches and a soft collar for a week and was back to normal.
23. Back Again
I was 18 years old and had just received delivery of a new motorcycle and rolled out of the dealership. A driver had fallen asleep and drove through the highway barrier into the service road which I was on and then into me. I saw it coming and braced, and somehow survived. About a month later, I took delivery on my second motorcycle to promptly get rear-ended at a red light by an inebriated driver.
Then at the end of the year, I got into an abseiling accident where a poorly anchored sling had dislodged and added additional rope to the line and jarred my back. I went to the hospital and had the same doctor again. His jaw dropped when he saw me. He straight up said, “How the [heck] aren't you dead, and why are you back”?
24. Back From Beyond
There was a patient who went into cardiac failure on the hottest summer day. He was found unresponsive for God knows how long, and a bystander started CPR. When the medics came, they did CPR for 29 minutes, and at the 30-minute mark, they found a pulse. He was taken to the ER and then transferred to the ICU. Once the patient "stabilized", the patient was transferred to our unit.
He was a complete vegetable, but the family did not want to pull the plug. He was unresponsive for a total of eight weeks, then one day, he woke up, and we found him on the floor trying to crawl out of his room. He pulled out his trach, lines, etc. He was so confused, and it was difficult to redirect him. At the time, it was pretty evident he had suffered severe brain damage.
Five weeks later, the patient was discharged from the hospital, mind fully intact, having passed all of the cognitive tests, etc. The patient told us all the events prior to his coronary. He said he received a second chance, and he wasn't going to mess it up this time. I'll never forget that patient.
25. She Was A Heartbeat Away From Death
I work in healthcare, taking ultrasound pictures of people’s hearts. I put my probe down on a middle-aged lady in the ER. I thought my machine was “frozen” and went to unfreeze the picture. It turned out her heart was barely beating, and it looked like it wasn’t moving. She had walked off the street and felt out of breath. A normal heart ejection fraction (how well it’s squeezing) is 55% and up. Hers was about 2% if that.
Because it was barely beating and blood wasn’t moving around, the blood started to clot together. It made a HUGE clot. It was an easy 6 cm x 5 cm. For reference, a female heart is considered to be dilated at 5.3 cm, so the clot inside the heart was bigger than a dilated heart. It was bad. I honestly have no idea how she was able to walk around at that point.
26. Low And Behold, She Was Walking
When I worked as a lab tech at a hospital in Connecticut, we had a patient come in complaining of weakness and dizziness. We ran a test called a CBC, as the doctor ordered. In doing the CBC, our machine wouldn't calculate the hemoglobin because it was so low. We had to use our blood gas analyzer to get a result. It was 2.8. The patient should have been passed out hard, but she wasn’t. She had walked in on her own.
27. Getting Buzzed For The Buzz
We had a patient who had a chronic PSVT (fast heart rhythm) who would eventually go into VT (a fast, irregular, unstable heart rhythm that will end you) and needed to get shocked to get back to a functional rhythm. He was basically "coding" while awake and needed to be defibrillated, or he would lose his life within a minute or two.
Chemical conversion (IV heart-stopping/restarting medication) didn't work on him for some reason. He REQUIRED defibrillation. VT is an ineffectual heart rhythm. It is not conducive to life. PSVT and SVT are like their precursors or predictors, so to speak. Your heart can only do PSVT/SVT for so long until it says, "All right, I'm out", with a last little run of VT. Then you’re gone.
Defibrillation HURTS. If you are conscious, it is not a good time. We sedate you with benzos (Versed) before we shock anyone because of this. This guy was also a substance user. He would stop taking the meds that kept his heart rhythm regulated just so he could come into the ER, where we didn't have time to debate whether we should give him benzos or not. We had to defibrillate him, and soon, or he'd go into VT and be gone.
The first three or four times, he got Versed. After that, the doctors figured out his game and shocked him without it. He played around with his own heart just to get a buzz, and he did it so many times he really should have been gone. I don't know how exactly he was timing it to be in the ER when he needed to be, or maybe he was just walking around in PSVT all the time without actually going into VT, but it just seemed like he should have perished SO many times.
He did it so much in the span of a couple of months that they ended up putting a pacemaker in him. The oral medications he took slowed his heart rate down effectively or maintained a regular, effective heartbeat once he was defibrillated. A pacemaker wouldn't have been required if he would have just continued taking his medications. But they put a pacemaker in him so that he couldn't manipulate his heart rhythm in an effort to get IV meds anymore.
Add to that the fact that any time we defibrillate, there's a small chance your heart won't start back up. Defibrillation isn't like a jump start. It's like getting hit by lightning. We really are interrupting the electrical conduction in your heart so that it resets itself. The dude was playing Russian roulette with his life, and any of those times could have ended him.
28. Back With A Vengence
I had extensive osteomyelitis in my foot from an infection the year before. I had done 89 days of outpatient IV Vancomycin for a MRSA infection, and I was in heavy denial that the infection had returned. Due to the necrotic bone, I had been told when the infection returned, not if. I was sleeping about 20 hours a day and could barely function.
Finally, after my wife threatened to divorce me if I didn’t act, I went back to the outpatient clinic to go back on IV meds. I rode there on my motorcycle—in the rain, no less—and went through the ER to get back into the outpatient program. The first thing they noted was my pulse oximeter readings were 68; they usually start freaking out at anything under 90.
Next, my blood pressure crashed to 78/42. I was rushed by ambulance to a major hospital and found to be septic and in early-stage organ failure. I vaguely remember an ER nurse who was very nice to me, but it was mostly a blur. Two weeks later, they amputated my right leg. A couple of days later, a nurse came to visit me to tell me I was the politest corpse who ever passed through her emergency room, and she was happy to see me on the road to recovery.
29. He Just Scraped By
Probably the craziest patient I had was during residency. I took a call about a patient with a slug wound to the center of his forehead, but they said he was talking and just complaining of a headache. EMS said it was witnessed by bystanders, and the guy had been blasted from a range of about ten feet. The guy showed up and had a crater in his forehead, an exit wound in the back, and this weird ridge that was really tender over his scalp. It was a sight to behold.
He otherwise said he was fine and just said he was sore. It turned out on his CT scan that the slug tumbled and basically followed the contour of his skull, and it was all superficial. It was a weird feeling to discharge someone from the emergency department who was blasted in the head.
30. A Long Road To The End
I was a nursing student and a nursing assistant at a hospital. We had a patient who came in with a blood clot in her leg from taking too much smack and passing out in a position where her leg was pinched beneath her. She was presumably found after almost two days, somehow still breathing. The clot in her leg formed while it was pinned awkwardly beneath her.
This patient was with us for almost six months. Normally patients are there for about a week, give or take a few days. During her six-month stay, she was losing weight drastically as she refused to eat. Her hair was matted and had to be cut off after many attempts to comb out the matting. She was probably 5’6” and was now down to 90 pounds.
She refused to participate in her physical therapy almost every day. She just didn’t want to get better, but was also very manipulative with the clinical staff, like only wanting pain medications but refusing to even have her vitals taken. Physical therapy pushed her every day, and some days were successful in getting her out of bed.
After she was strong enough to walk with a walker and the blood clot had been treated, she was discharged to a shelter downtown. Within 24 hours, she went to the ER at another hospital, and they sent her back to us. She stayed another eight months with us, with her same old ways—refusing care and not eating. By the time she finally passed, she was 68 pounds and had basically starved herself.
She refused any feeding tubes and, basically, any help the clinicians suggested she denied. I don’t think she would have even lived that long if it weren’t for the IV fluids. She was seen by a psychologist many, many times and would refuse their help as well. She looked like she was already gone from the moment she came in. I just couldn’t believe she was a resident at our hospital for over a year before she finally passed.
31. She Must’ve Had Nerves Of Steel
My cousin, who’s a doctor in our country, told us about a freak accident involving a pregnant patient. She was rushed to their hospital because her belly was pierced by a falling steel rod from a top of a construction site while she was riding a motorcycle with her husband at normal driving speed. She was brought to the hospital with the rod still pierced through her. It was truly horrifying.
They had to saw the rod out and deliver the baby immediately after. Luckily, no vital organs were damaged, and the baby was in the right position inside the mom’s belly at the right time. Therefore, it survived and was delivered safely.
32. Saved By A Sliver
A "regular" came into the ER one night. He was a heavy drinker, a petty thief, and habitually got into trouble with his friends and business associates, ending up in the ER on a semi-regular basis for falling over, fighting, or some other idiocy. He was about 50 years old. This time he owed a "friend" some money, so there was a collection call.
Not one to have much money at home, it ended in an altercation, and he was knocked to the ground, after which the "friend" put a foot on his neck and hit him in the temple with a crowbar before leaving him bleeding on the concrete floor. The regular’s guest called the ambulance, which shipped him in. He was fully ambulatory, meaning he could walk and was coherent.
He wanted to grab some smokes and eat snacks and didn't really understand why he was in the ER. Indeed, he only had some slight swelling, could use both eyes and had no real pain. However, we decided to X-ray him, and I wheeled him up. He insisted on getting on the X-ray bed by himself, but we didn't let him get up by himself. It looked like a horror show. The side of his head was completely crushed into little bits, and a major blood vessel was torn open.
However, he got a one-in-a-million break, and one of the small shards of bone was lodged into the torn blood vessel, just about sealing it. Without that, he would have been long gone before his guest got through to emergency services. He was immediately shipped to emergency services and came down to visit and buy snacks two days later, completely recovered. He was millimeters from losing his life, with just pure luck saving it.
33. Everything Was NOT Fine
When I was 30, I survived two episodes of ventricular fibrillation before they figured out what was happening and put a defibrillator in my chest. When they put the ECG on me after the first episode, they thought the machine was broken because my heartbeat was so irregular. The second episode was caught on an implanted monitor.
The next day when they downloaded and read the results, the technician thought his machine was broken. Then his face froze, and he said, "Don't worry, everything is fine”! As he ran out of the room to get the cardiologist, I yelled back that, "It seemed like everything was not fine"! I had a defibrillator implanted about an hour later. I've had three ablations since then, and so far, I'm still here.
34. Sick To Her Stomach
When my wife was still in medical school, she had a teenage patient while she was on a family practice rotation. A girl came in who was complaining of awful pain for a week and a half. Her parents said she's usually not a complainer but ignored it anyway. My wife tried to convince her attending that it was appendicitis, but the attending said it had been too long for appendicitis.
My wife finally convinced the attending to get imaging done. The girl was walking around with a ruptured appendix for one and a half weeks. Apparently, her stomach cavity was full of infection, and she had clots in her arteries. Once discovered, the parents still didn't want to take her to the ER. However, eventually, they took her to the ER.
35. Waiting Game
The first time I witnessed a pulseless V-tach (ventricular tachycardia) patient, he probably did have a pulse and was just super weak, but we couldn't feel one. The guy was awake with no complaints other than being cold. He was as pale as I had ever seen a human, and he was that way for two hours before we got a cardiologist in.
We cardioverted him a few times, which is similar to using a defibrillator but has some specific criteria. But we didn't want to sedate him too much with Ativan because it was better if he didn’t go to sleep. We all hovered around his room, waiting for him to pass out finally so we could start CPR, but he never did. He just kinda hung out and watched Wheel of Fortune, waiting to literally perish.
36. Totally Blocked Out
My father was getting a lot of tests done for his heart, which had been giving him some trouble. The doctor showed him the test results, a diagram of his heart and the major arteries, along with how blocked each one was. The best one was 90% blocked, and the worst one was 100% blocked. The doctor said, "Frankly, I'm not certain how you're sitting here having a conversation with me".
Quintuple bypass surgery followed. He's still alive two years later and got to meet his first grandchild. We keep a copy of the test results around as a reminder.
37. My Numbers Were Off The Charts
Circa 2013, I was 466 pounds of goo, had mega diabetes, and was 29 years old. I had no job by choice, no friends by choice, and no life by choice because World of Warcraft had me by the nuts. Years later, around 2019, I had been progressively losing weight, hovering around the 230ish mark, when I started to get pains in my no-no place at times when I was not actively using said body part.
I had woken up in the middle of the night to what felt like a lightning bolt striking the peduncle of my schlong. I went to the doctor, and they wanted to check if I stuck my wang in a cesspool, so they sent me for bloodwork. I got woken up that night at 4:30 AM by my phone. Somehow the ringer pushed through the “do not disturb” mode despite me not having any types of bypasses on it.
The doctor I went to see that day was on the phone and said my blood work resulted in a red flag alarm, meaning a life-threatening problem. Normally finding cancer and whatnot is what causes this. My glucose was off the charts. A non-diabetic should be between 1–5, subjective to which Endo you speak to. A well-controlled and good type 2 diabetic should have blood glucose around 4–7.9.
Anything between 8–12.9 is high, and you need to go drink some water, and 13–19.9 is critical, you have to go to the hospital. Anything over 20 generally results in extreme trashed-like behavior where you are unable to walk, sometimes unconscious, and have a loss of bodily functions, etc. At the time of withdrawal, my glucose measurement was 44 at roughly 9:30 AM, and I hadn’t eaten anything or drank anything yet that day.
The doctor told me to hang up and call for an ambulance. Don't drive myself there, don't get a family member, it was time for emergency services. So, I drove myself over to the hospital. This was roughly 5 AM the next day, and my blood was measured again. It was 48. The doctors checked it three times, with three different blood draws, and gave me three bags of IV fluids between draws.
Yet, I was consistently at "you should be no longer alive" high numbers. When I fast forward to last month, I am now around 160 lbs, and my A1C averages at a 7, so very well-controlled and medicated.
38. A Cocktail Of Conditions
When I was 25, I was sick at home for two weeks. I had visited the ER three separate times, and since this was right before Texas got slammed with COVID, they just assumed it was COVID-related and didn’t really do anything for me other than also diagnose me with strep. The antibiotic I had received didn’t work. I had bad fevers on and off that eventually stopped breaking.
On my third ER visit. I checked in at the COVID check-in. I had a temperature of 104°F, my O2 was 79% (normal is >94), and was sent to another ER for a higher level of care. I was septic from parainfluenza, m.pneumonia, strep, and Rocky Mountain spotted fever. I basically went into multiple organ failure, and my kidneys got it the worst.
I actually went into cardiac failure shortly after being intubated in the ER. I survived all of that thanks to dialysis and woke up in the ICU three to four days later with no memory of anything. I actually am an RN and worked in the same ICU a year later, and all my coworkers said they thought I was going to be a goner at any minute.
39. Everything But His Brain Was A Bust
I had a patient who blasted himself in the head but only managed to destroy all of his suborbital structures (everything below his brain). His eyes were mostly destroyed, but the remnants were falling down into what used to be his mouth. Other than that, he had a bunch of destroyed muscles and ligaments and blood dangling down from his maxilla.
To intubate him, we just put the tube directly in what was left of his larynx. You could see the gas bubbling through the blood. We later converted it to an actual tracheostomy. Obviously, I couldn’t tell how he was doing, but he was thrashing around, breathing really quickly, but no longer able to scream because his larynx was essentially destroyed. I think he must have eventually passed, but who knows?
40. This Patient Bowel-ed Me Over
A liver transplant patient came in with a closed-loop small bowel obstruction that she had ignored. Basically, a foot-long segment of her gut twisted on itself at both ends due to adhesions from her transplant surgery, so it resembled a link sausage. This cuts off the blood supply. She came in about three days after that. The bowel had perished, and she had a necrotizing infection of her abdominal wall.
Because of her immunosuppressives, her body hadn’t really mounted an immune response. There was a hole leaking pus about 8 cm above her umbilicus. She was told she would likely perish whether or not we operated, and she chose to try. She coded twice on the OR table and ended up having a fist-sized portion of her abdominal wall and two feet of small bowel excised.
She went to the ICU intubated with an open abdomen and basically a sheet of iodine-infused Saran Wrap holding her insides in. Over the next three months, she went to the OR four more times for further debridement until she basically had no abdominal wall left. Two weeks before she passed, I vividly remember how horrifying it was to see her consciously sedated with a breathing tube in feeling her bowels under the iodine wrap. It was the most surreal thing ever. She passed two weeks later from sepsis.
41. Pandemic Patients
During the first wave of COVID in the US, I was a paramedic who worked in Queens when it was the epicenter. We’d get inundated with calls—over 6,000 a day—which was two times our daily average, and it was nuts. It got so bad we had a protocol in place to leave you at home if you weren’t that sick. One of the moments that stuck with me about how bad this was going to be, was when I got to a 48-year-old woman in her apartment.
She called because she felt unwell. My partner and I were shocked at the gall of this woman to call for an ambulance in the middle of a pandemic when hospitals were at capacity because she felt “sick”. She looked uncomfortable but otherwise fine. My partner and I were getting ready to deem her safe to stay at home when I decided to put the pulse oximeter on her for a complete vital signs assessment, and she had a saturation of 51%.
I didn’t think the machine could go that low. I looked at her, and she seemed sick but not critical. It didn't make any sense. I got another pulse oximeter, and it had an identical reading. I checked it on myself and my partner, and it was in good working order. I put it in all of her fingers, and again 51%. I looked at her again, and she was completely alert and oriented, with full decisional capacity and normal breathing.
Her lung sounds were immaculate. I couldn’t believe it. Most healthy people with no pulmonary issues have severely altered mental status and confusion when their saturations are in the high 80s. She was hanging in the 50s. With supplemental oxygen via a mask, I got her as high as 84%. This woman, for all intents and purposes, was cognitively at her norm and looked as if she may have had a stomach bug.
But in reality, she was beyond hypoxic and critically ill. We knew nothing about COVID then and seriously debated intubating her, but seeing how comfortable she appeared and how she wasn’t working hard to breathe, we decided to leave her be and just transport her to the hospital. I started an IV on her, and I felt my face go pale. I watched as the hub of the angiocatheter (the plastic holder of the needle I use to start an IV) started filling with the darkest, blackest blood I’d ever seen in my entire life.
It looked like chocolate syrup. It was then I realized we were in serious trouble, and this was just the beginning. That oxygen saturation, in conjunction with other signs, symptoms, and story, would ultimately be the big indicator at the time of how sick you were and had a high degree of success in indicating if you had COVID.
The lowest saturation I’d eventually see in a COVID patient would be in a 32-year-old guy who met me at my ambulance. He literally walked to my truck with a saturation of 42%. He looked like he felt sick, but again nothing about his appearance screamed he was dying inside. It’s been almost two years, and I’ll never forget it.
42. She Couldn’t See How Lucky She Was
In my ophthalmology residency, I was called in to see a young woman. She was at home when someone came looking for her boyfriend, who was not there. The man held a piece to her left temple and pulled the trigger. The slug entered the left temple on a path going from posterior to anterior, completely severed her left optic nerve, went across the nasal cavity, and obliterated her right eyeball before exiting, leaving her totally and irreversibly blind.
It stayed under the cranial vault, and as I was assessing her, she was awake and completely lucid and able to answer all questions. We tried to piece together what we could to save the right eye, but eventually, it had to be removed. She was the luckiest unlucky person I have ever come across.
43. He Had Been Through It All
When I was a student physiotherapist, I did a placement at a hospital, where I would basically work with inpatients who were gaining strength to be discharged; basically, bed exercises post-surgery, working up to taking steps, then walking independently. It was pretty simple stuff. Whenever I had a new patient, I would be given a full patient report with their entire medical history.
Usually, they were anywhere from three to six pages long and very thorough. One time, I was told I had a new patient, and the report was on the reception desk. I went looking for it, but couldn't find it. The reason was that this report was not a couple of pieces of paper stapled together but instead a binder—it was 48 pages long.
The patient was in his 90s, been through two wars, multiple car crashes, heart failure, stroke, diabetes, lost limbs, bladder infection, dementia, etc. You name it, he had it. Under the "goals" section was a sort of generic "return to walking and regain independence". I met him once, and, well, that was just never gonna happen.
I did a few bed exercises with him and helped train him to sit up by himself, but that's about as far as we got. He didn't make any real improvements; eventually, he was labeled palliative. He lasted my entire placement, still alive by the time I left. Just the absolute definition of a tough dude.
44. From Mummy To Man
I saw a guy who effectively had an explosive go off in his face. Something about welding and igniting the air around him (like a gas leak.) A co-worker pulled him out, and the guy “walked” over a few steps to the helicopter before collapsing. He was young, and I first saw him earlier in his recovery in the burn unit. His co-worker was there, too, for burns on his leg.
The patient had head-to-toe burns and corneal burns too. I saw him again a few months later and didn’t realize it was the same patient until a couple of hours into my shift. I didn’t know before, but he had green eyes and bright red hair. He was talking and able to sit up and eat. He had been there for months. Seeing someone completely covered in bandages progress that much was incredible.
45. Defying The Odds
I work in home care, and we just took on a new client. She's 88 years old, has COPD, and has been on 24-hour oxygen for at least a year. Four months ago, her husband of 60 years passed. She got COVID, COVID pneumonia, blood clots from COVID, then bacterial pneumonia. Any one of these things should have done her in, considering her age and the COPD.
She really hasn't even been able to grieve the loss of her husband. But here she is, finally at home, awake and alert and needing some basic companionship and caregiving because she lost a lot of strength and endurance while hospitalized. She's smart, funny, and fairly independent, and I'm really glad we get the opportunity to help her.
46. Granny Wasn’t About To Go
I was a paramedic and got called for a coronary. A 90-year-old woman had been down on the back porch for an unknown time. Her medical history was a mile long. The monitor showed asystole (flatline), and her extremities were starting to get cold. Her core was still warm, and the family swore she was fine ten minutes prior. So, by our protocol, she was still viable, and thus, we started to work on her, but it seemed obvious she was gone.
The entire code was a mess. It took forever to get an IV, her airway was full of vomit, and the suction device didn't work. An intubation attempt went into the stomach. The rookie dumped out the meds box—it was terrible. We worked on her for a half hour with no change. The woman was gone. We called the hospital and received orders to end resuscitation.
We explained to the family that we'd done all we could but that grandma had perished. We then stopped CPR. As soon as we took our hands off the woman's chest, the monitor showed a rhythm. We checked for a pulse, and it was bounding. We loaded the woman into the ambulance, called the hospital to say “just kidding” about the pronouncement, and screamed off to the hospital.
Normally when we get pulses back after a cardiac case, we're just bringing back a vegetable. The percentage of people who actually leave the hospital with any kind of quality of life is minuscule. Most of the time, they just sit in the ICU for a few days and then lose their life again permanently. Not this woman. A few months later, we get called out to the same address and find the same woman sitting on the couch. She had some deficits and memory loss and needed a wheelchair, but she was alert and home with her family. It was the strangest thing I ever saw.
47. It Was Almost The Nail In His Coffin
We had a patient come in after mowing the lawn. The patient said something was knocked up by the lawn mower and hit him in the head. He didn't think much of it and finished cutting the grass. He still had a headache a few hours later, so he came to the ER. We CAT scanned his head, and there was an entire nail embedded in his brain. He had the tiniest abrasion to his forehead and no neuro deficits. He had no idea. Everyone was absolutely dumbfounded.
48. He Was On A Slippery Slope
My ex-boyfriend is a ski instructor. He told me that one day, all the slopes were extremely icy, and many people were coming in with injuries. He had fallen badly and returned to the ski lodge. He was checked out and said he felt fine. Fortunately, a paramedic happened to be looking at him when his helmet swung open on the side because it was very badly cracked.
They took a nine-year-old girl with a broken femur off a stretcher and put him on it, and took him to the hospital immediately. They found he had broken his neck and needed immediate surgery. Amazingly, he is mostly fine, except now he has acid reflux for some reason.
49. His Life Was Almost Shattered
I was a paramedic. There was a patient who had shattered their spine by falling off a six-story building. They weren’t trying to hurt themselves but were hanging out on the roof. He had immense internal bleeding and a nasty concussion, but the impossible part was that he nearly shattered all his spinal bones, but his spinal cord was intact. I still see him from time to time, he was in a full-body cast for five or so years, but from my knowledge, he is doing fine and has two kids and a wife.
50. Life Was Squeezing By
My mom was an ER nurse right after college. A family got in a car crash, and there weren’t any serious injuries; they were just taken to the ER to be assessed. They had a baby, and my mom was asking them questions about its health, etc. When she asked what the baby was being fed, the mom said, “Juice”. Just juice. She had heard that at six months, you could start feeding the baby juice, not realizing it was juice, in addition to baby food or milk. This woman had been feeding her baby ONLY JUICE for months.
Sources: ,